Coronary artery disease: what causes it and how to act fast
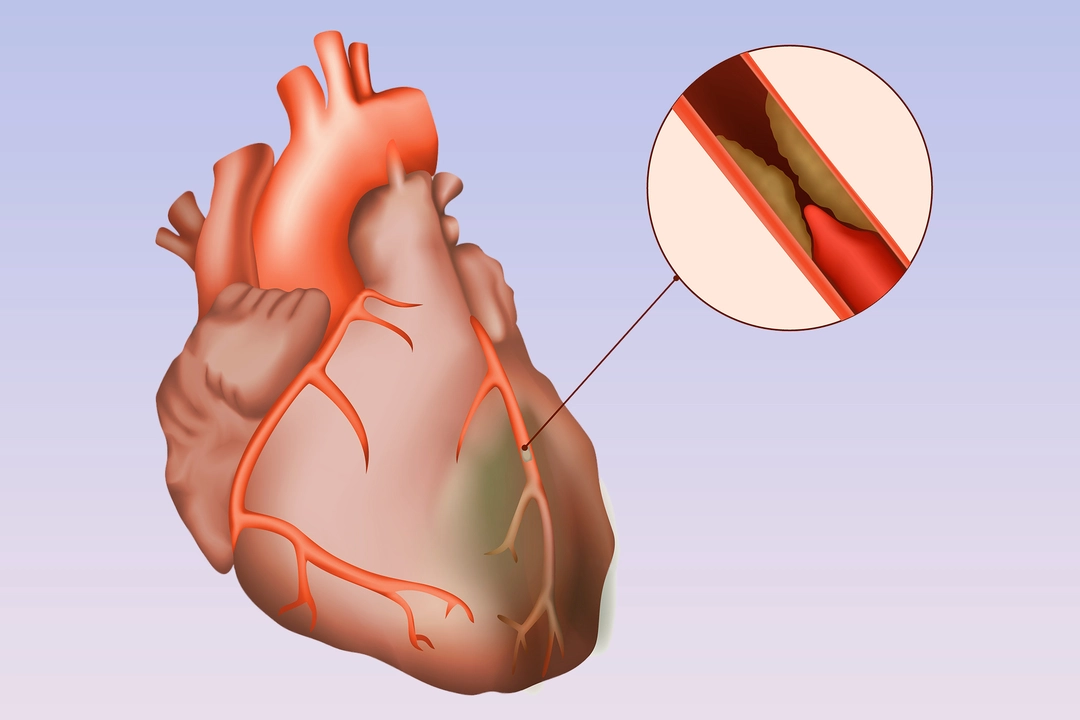
Coronary artery disease (CAD) means the arteries that feed your heart have fatty buildup. That plaque narrows the vessel and reduces blood flow. You may not feel anything at first, but over years that narrowing raises your risk of chest pain, heart attacks, and shortness of breath.
Here’s a direct, useful look at what to watch for and what you can do right away.
Common causes and clear warning signs
Major drivers of CAD are high cholesterol, high blood pressure, smoking, diabetes, being overweight, and a family history of early heart disease. Age and male sex raise risk too, but lifestyle makes a big difference.
Warning signs range from subtle to urgent. Classic signs: pressure or tightness in the chest that may spread to the arm, jaw, or back; shortness of breath; sweating; nausea; or sudden fatigue. If chest pain lasts more than a few minutes or is severe, call emergency services right away.
Tests, treatments, and simple steps that help
Your doctor will likely start with a resting ECG and blood tests for cholesterol and sugars. If needed, you may get a stress test, coronary CT angiography, or invasive coronary angiography to map blockages. These tests guide whether you need medicines, a stent, or bypass surgery.
Medications that reduce risk and symptoms include statins to lower LDL cholesterol, aspirin or other antiplatelet drugs to reduce clots, and medications to control blood pressure and heart workload (beta-blockers, ACE inhibitors or ARBs). Nitroglycerin helps with short-term chest pain. If a blockage is severe, a cardiologist may recommend stenting (PCI) or coronary artery bypass grafting (CABG).
Daily habits matter. Quit smoking — within months your heart health improves. Aim for 30 minutes of moderate activity most days: walking, cycling, or swimming count. Focus on a diet rich in vegetables, whole grains, lean protein, and healthy fats (think oily fish, nuts, olive oil). Keep weight and blood sugar in check. Small changes add up: swapping soda for water, walking after dinner, and cutting down on processed snacks are easy wins.
Monitoring matters. If you’re on statins or blood pressure meds, do follow-up blood tests and clinic visits. Track numbers: LDL cholesterol, blood pressure, HbA1c if you have diabetes. These are practical measures that tell you if the plan is working.
If you have questions about medicines, tests, or how to lower your risk, bring specifics to your healthcare provider. Ask what your actual risk score is and which single change would give the biggest benefit for you. That makes the plan realistic and focused.
Coronary artery disease isn’t a sentence. Many people live well for years after diagnosis by combining meds, smart lifestyle moves, and timely care. Start with one concrete change today — quit smoking, move more, or ask your doctor about a cholesterol check.