Blood Cancer: Signs, Types & Treatment
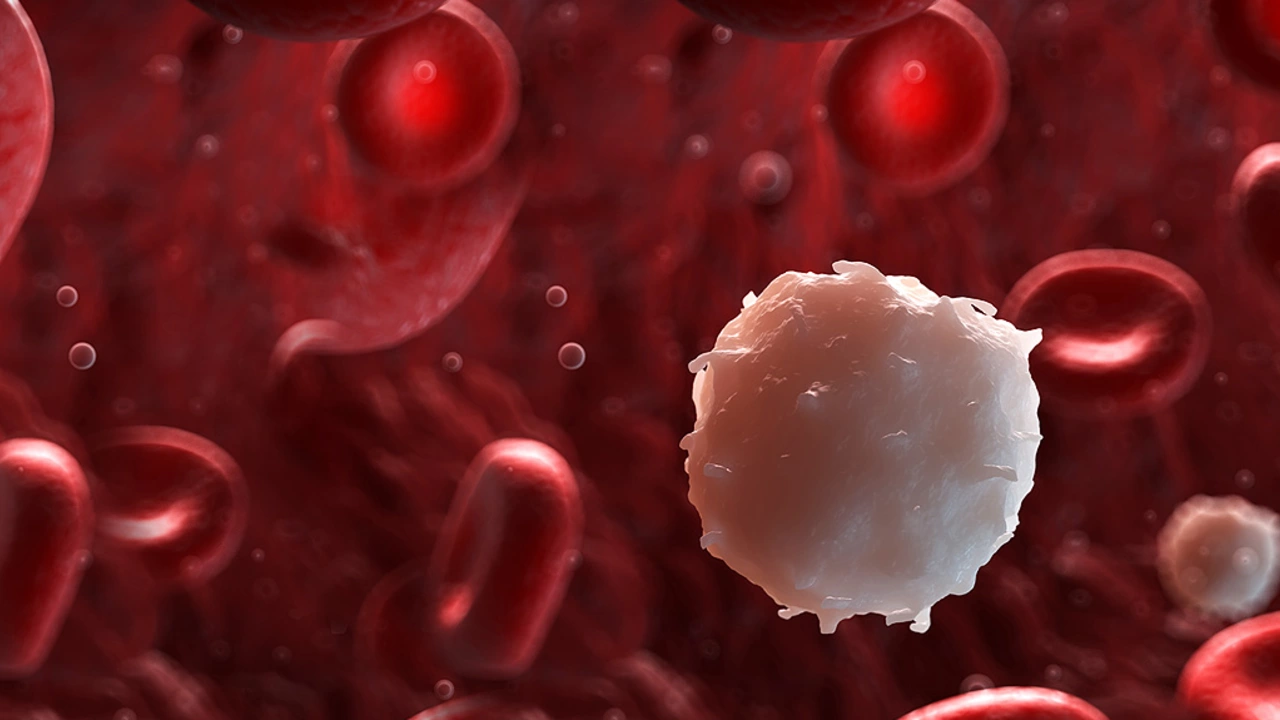
Blood cancer is not one disease — it's a group of cancers that start in the bone marrow or lymphatic system. You might hear the words leukemia, lymphoma, or myeloma. Each behaves differently, but all affect your blood, immune system, or how blood cells grow.
Noticed sudden bruising, frequent infections, unexplained weight loss, night sweats, or swollen lymph nodes? Those are common warning signs to check out with a doctor. Fatigue that won’t go away and shortness of breath can also mean low red blood cells. None of these symptoms prove cancer, but they’re signals that need testing.
How blood cancers differ
Leukemia usually starts in bone marrow and floods the blood with abnormal white cells. Lymphoma starts in lymph nodes or tissues that fight infection. Myeloma affects plasma cells and can weaken bones and kidneys. Treatment and outlook depend on the specific type, how fast it grows, and your overall health.
Doctors use blood tests, bone marrow biopsy, and imaging (CT or PET scans) to pin down the diagnosis. A pathologist will look at cell types and genetic changes. Those genetic details matter: they guide treatment choices and give a clearer idea of prognosis.
What to expect from diagnosis and treatment
Treatment options today go beyond standard chemotherapy. Targeted drugs attack specific genetic faults in cancer cells. Immunotherapy helps your immune system recognize and kill cancer. Radiation treats specific areas, while stem cell transplant can replace damaged marrow after high-dose chemo. Your team may mix approaches to get the best result.
Side effects are real: infections, hair loss, nausea, fatigue, and low blood counts are common. Ask your team about growth factors, anti-nausea meds, and infection prevention. Many side effects are manageable, and supportive care can make treatment more tolerable.
Practical tips: bring a list of current medications and allergies to appointments, write down questions before visits, and ask for plain explanations of test results and treatment goals. If you’re deciding between options, ask how each affects daily life, fertility, and long-term follow-up.
Follow-up matters. Even after successful treatment, the team will watch blood counts and organ function for years. Some treatments raise risks for other health issues later, so regular check-ups help catch problems early.
If you’re the caregiver, help with medication schedules, track side effects, and keep a record of appointments and lab results. Emotional support for patients and family is important — counseling or support groups can help you cope with stress and decisions.
Questions to ask your doctor right away: What type of blood cancer is this? What tests do we need? What are the treatment goals? What side effects should I expect, and how will they affect daily life? Who coordinates my care?
Blood cancer is a serious diagnosis, but treatments have improved a lot. Getting clear answers, a plan, and a support team makes a big difference. You can also ask about clinical trials, second opinions, and financial help programs — these options sometimes open better choices for more support.