Understanding Azathioprine and Its Uses
Azathioprine is a widely used immunosuppressive medication that belongs to the class of drugs called purine analogs. It works by inhibiting the synthesis of DNA, RNA, and proteins in cells, thus suppressing the immune system. Azathioprine is primarily used to prevent organ rejection in transplant patients and to treat autoimmune diseases such as rheumatoid arthritis, lupus, and Crohn's disease.
As with any medication, there are potential side effects and risks associated with azathioprine use. One of these risks is the increased susceptibility to infections, particularly pneumonia. In this comprehensive review, we will delve deeper into the risk of pneumonia in patients taking azathioprine and discuss the various factors that contribute to this risk.
How Azathioprine Increases the Risk of Pneumonia
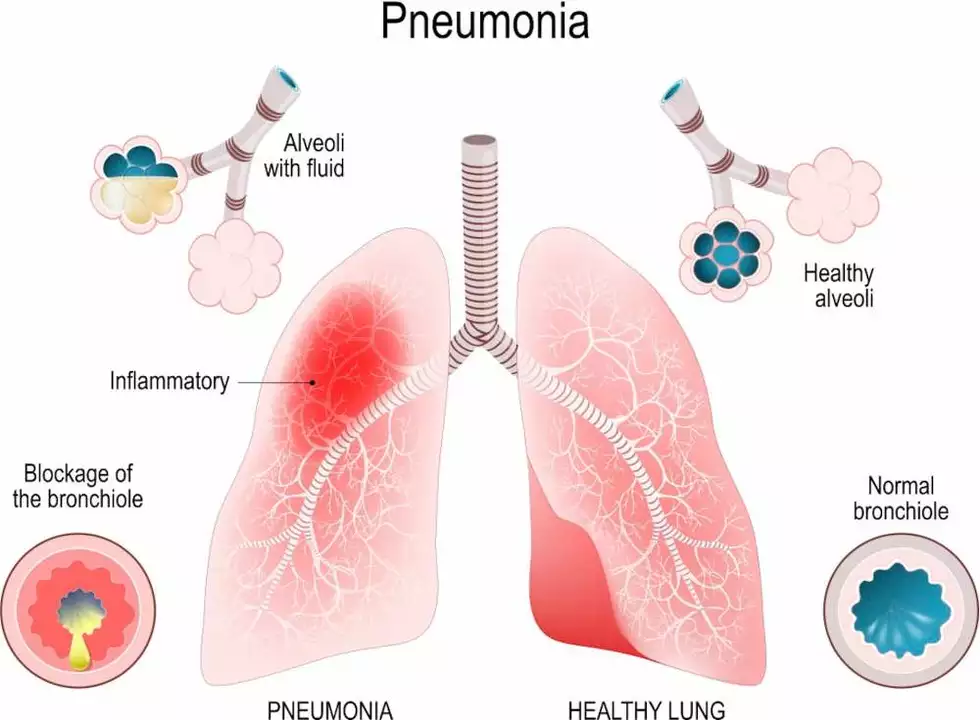
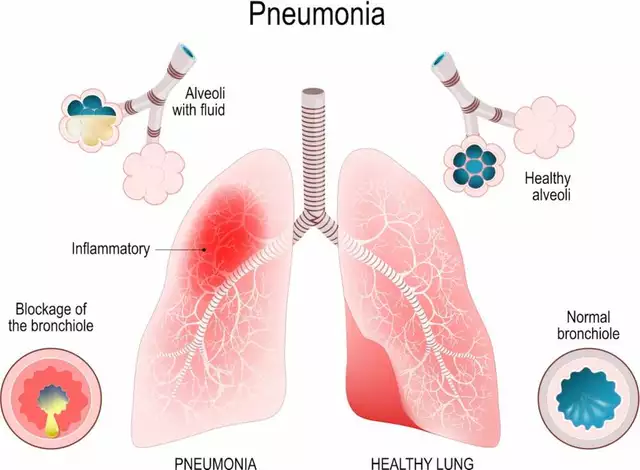
Given its immunosuppressive properties, azathioprine can leave patients more vulnerable to infections, including pneumonia. Pneumonia is an infection of the lungs caused by bacteria, viruses, or fungi. The immune system plays a crucial role in fighting off these pathogens and preventing infection. However, when the immune system is weakened by medications like azathioprine, the body's ability to combat infections is significantly diminished.
Patients using azathioprine are more susceptible to opportunistic infections, which are infections that take advantage of a weakened immune system. These opportunistic pathogens, such as Pneumocystis jirovecii, are usually harmless to people with healthy immune systems but can cause severe pneumonia in immunosuppressed patients.
Factors That Affect the Risk of Pneumonia in Azathioprine Users
Several factors can increase the risk of pneumonia in patients taking azathioprine. These include the patient's age, the presence of other underlying health conditions, and the dosage and duration of azathioprine treatment.
Older adults are more likely to develop pneumonia due to their naturally weaker immune systems and a higher prevalence of underlying health conditions. Patients with chronic lung diseases, such as chronic obstructive pulmonary disease (COPD) or asthma, are also at an increased risk of pneumonia, as their lung function is already compromised.
The risk of pneumonia may also be higher in patients who are on higher doses of azathioprine or who have been taking the medication for a longer period. This increased risk is due to the cumulative immunosuppressive effect of azathioprine over time. It is essential for healthcare providers to carefully monitor patients on long-term azathioprine therapy and adjust the treatment plan as necessary to minimize the risk of pneumonia.
Preventive Measures to Reduce the Risk of Pneumonia
There are several preventive measures that can be taken to reduce the risk of pneumonia in patients using azathioprine. These include vaccination, prophylactic antibiotic use, and maintaining good hygiene practices.
Vaccination against pneumonia-causing pathogens, such as Streptococcus pneumoniae and Haemophilus influenzae, can help protect azathioprine users from infection. In addition, it is essential for patients to receive the annual influenza vaccine, as the flu can lead to secondary bacterial pneumonia.
In some cases, healthcare providers may prescribe prophylactic antibiotics to prevent pneumonia in high-risk azathioprine patients. However, this approach should be used with caution, as the overuse of antibiotics can contribute to antibiotic resistance and the development of drug-resistant infections.
Maintaining good hygiene practices, such as frequent handwashing and avoiding contact with sick individuals, can also help reduce the risk of pneumonia. Additionally, maintaining a healthy lifestyle, including regular exercise, a balanced diet, and adequate sleep, can help support the immune system and overall health.
Conclusion: Balancing the Benefits and Risks of Azathioprine Use
In conclusion, azathioprine is a valuable medication for many patients with autoimmune diseases and transplant recipients. However, its immunosuppressive effects can increase the risk of pneumonia and other infections. It is crucial for healthcare providers to carefully assess each patient's individual risk factors and closely monitor their health while on azathioprine therapy.
Preventive measures, such as vaccination, prophylactic antibiotics, and good hygiene practices, can help reduce the risk of pneumonia in azathioprine users. Ultimately, the decision to use azathioprine should be based on a careful evaluation of the potential benefits and risks, and patients should be educated about the importance of maintaining their overall health to minimize the risk of infections.





Post A Comment